Stem Cells: Ray of Hope for Retinitis Pigmentosa Patients
MRUNMAYEE DUPALLIWAR
DR. D. Y. PATIL BIOTECHNOLOGY AND BIOINFORMATICS INSTITUTE
mdupalliwar@gmail.com
‘Retinitis pigmentosa’ (RP) and age-related macular degeneration are eye diseases resulting in a gradual decline in a person’s vision. One in every 6000 people in the world is affected by RP. In both conditions, progressive dysfunction and death of light-sensing photoreceptors of the retina and other supportive cells occur. Initial symptoms include nyctalopia (night blindness) usually from adulthood followed by loss of peripheral vision and loss of central vision. Transplantation of progenitor stem cells which can be stimulated to replace photoreceptor cells may help restore visual function. Stem-cell based Retinal Pigmented Epithelium (RPE) transplantation is under trial.
Retinas have a centripetal proliferation of bone, spicule-like pigmentation and attenuation of retinal blood vessels in RP. Around 50 genetic mutations are responsible for such conditions, out of which the most common ones were found in the RHO gene which is responsible for production of ‘rhodopsin’ (a pigment-containing, sensory protein necessary for normal vision, especially in low light).
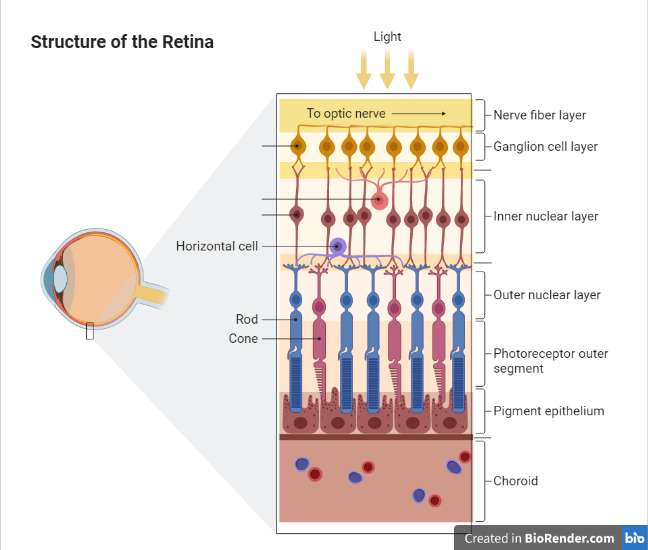
The outer blood-retinal barrier between photoreceptor cells and choroidal blood vessels is the RPE. Photoreceptor cells are functionally dependent on RPE. Mutation in any of the genes responsible for its function may lead to retinal degeneration. It can also be caused by inherited, physical or chemical damage resulting in gradual loss of RPE and photoreceptors.
Two types of stem cells i.e. embryonic and induced pluripotent stem cells may produce retinal progenitor cells. The mesenchymal stem cells derived from umbilical cord Wharton’s jelly were recently used for administration in sub-tenon space to study their beneficial effects on visual functions in RP patients by reactivation of the degenerated photoreceptors. 34 eyes from 32 RP patients of various genotypes enrolled in clinical stem cell research were included in the study. Significant improvement was seen in the visual field, retinal thickness values, after 6 months of application.
Mesenchymal stem cells (MSCs) are non-hematopoietic multipotent stromal cells isolated from bone marrow, adipose, umbilical cord, placenta, dental pulp, amniotic fluid, etc. MSCs derived from umbilical cord Wharton’s jelly (WJ-MSCs) are hypoimmunogenic, suppressing chronic inflammation, preventing apoptosis as well as stimulating progenitor cells for self-repair mechanism. WJ-MSCs are superior to other cell types as they are easily obtained and exhibit characteristic features like better tissue compatibility, rapid proliferation, long-term efficacy in transplanted tissue, high paracrine activity, no tumoral side effects and features similar to RPE. No immune rejection occurred as WJ-MSCs do not synthesize MHC II antigen. The sub-tenon region acts as a natural culture medium and provides immune protection.
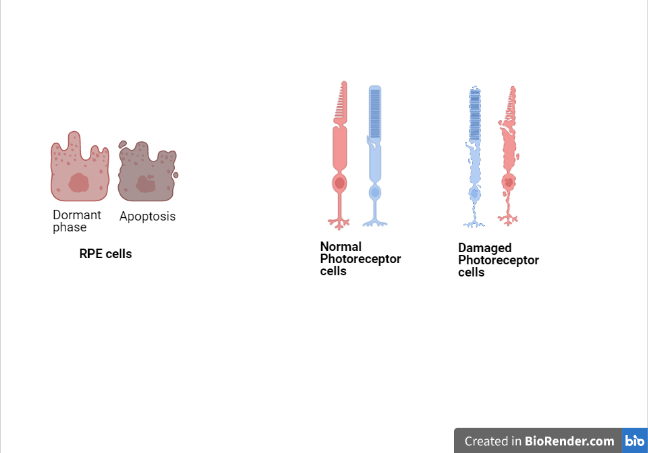
WJ-MSCs can proliferate faster than adult tissue (adipose) MSCs, as they’re isolated from neonatal tissue and undergo lesser nuclear and mitochondrial mutations. Their unique effect on activated macrophages reduces the secretion of inflammatory factors. Instead, factors supporting cell survival and regulation of adjacent cells in damaged tissue are secreted. Adipose MSCs can proliferate 5 times while WJ-MSCS can proliferate 25-300 times without karyotype changes. Therefore, the paracrine trophic effect of WJ-MSCs may stay for 3-7 years without needing frequent injections, unlike the case of adipose MSCs.
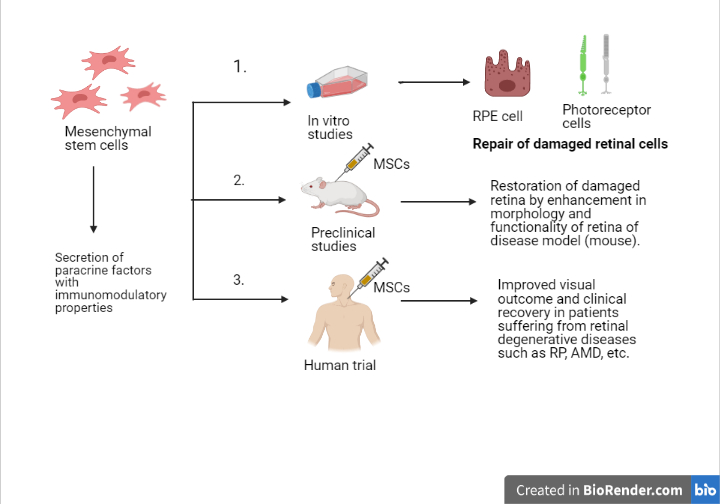
WJ-MSC therapy protocol
When the activity of growth factors decreases in the surrounding, photoreceptor cells come to rest (dormant phase) and further decrease leads to apoptosis. But growth factors (GF) secreted by MSCs such as neural GF, brain-derived neurotrophic factor, the ciliary neurotrophic factor can slow retinal degeneration. These factors help balance the microenvironment of cells, but the effect is local and short-lived. So, to ensure long-term action, MSCs produce exosomes containing microRNA, GFs, mRNA, etc. As a result, photoreceptors in the dormant phase may be reactivated, regenerating synaptic connections thus improving vision. Although, some research is still needed to determine the duration of efficacy and the intervals at which the WJ-MSCs administration will be required.
There are only a few treatment options to slow or stop the progression of this disease. Sub-tenon implantation seems to be a reasonable way to avoid severe side effects of intravitreal/ submacular injections. Thus, it is one of the most effective and safest options for RP treatment developed till date.
Reference (Apr-21-A7)
About the Author
I am a first year MSc Biotechnology student from Dr. D. Y. Patil Biotechnology and Bioinformatics institute. My aim is to work in stem cell and regenerative medicine and Environmental biotechnology. I was a part of Plastic Biodegradation project which was presented in Raman Science centre, Nagpur, in 2018. I am currently working on Helicobacter pylori infection. I wish to be involved in rigorous research and development in future to help create a better future for mankind in a sustainable way.

