Mesenchymal Stem Cells The future of Bone Regenerative Medicine
AYUSHI SINGH
DR. D.Y. PATIL INSTITUTE OF BIOTECHNOLOGY & BIOINFORMATICS
ayushidoc09@gmail.com
What are Stem Cells?
Stem cells are unspecialized cells of the human body that have the potential to differentiate into any cell of an organism. Stem cells also have the ability of self-renewal and excess proliferation.
Types of stem cells
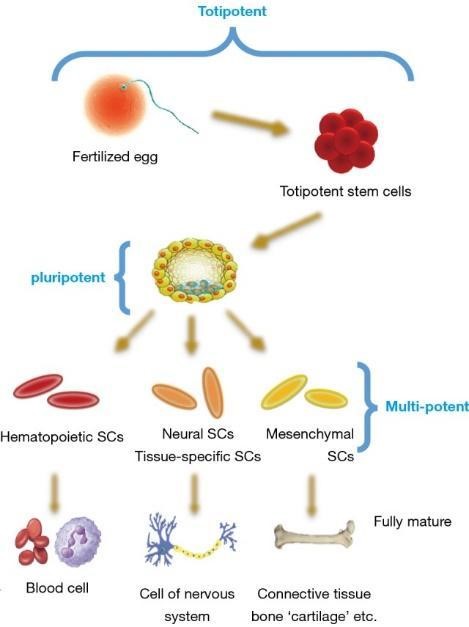
Based on their differentiation ability, Stem Cells are classified into:
Mesenchymal Stromal Cells (MSCs)
Mesenchymal Stem Cells (MSCs) are the type of cells with the potential of multi-lineage differentiation and self-renewal.
MSCs in Bone Regenerative Medicine
BONE REGENERATION – Bone is a unique tissue that could regenerate completely after injury rather than heal itself with a scar. Bone regeneration is a complex, physiological process of bone formation and is involved in constant remodeling throughout adult life.
There are some complex clinical conditions in which bone regeneration is required, such as for skeletal reconstruction of large bone defects created by trauma, infection, tumor resection and skeletal abnormalities, and also osteoporosis.
Current Therapeutic Strategy – Autologous Bone Grafting. Bone grafting is a commonly performed surgical procedure to augment bone regeneration in a variety of orthopedic and maxillofacial procedures, with autologous bone as it combines all properties required in a bone-graft material: osteoinduction bone morphogenetic proteins (BMPs) and other growth factors, osteogenesis and scaffold.
Drawbacks of the Current Treatment
- The limited supply of autologous bone
- Increased operation time and blood loss
- Temporary disruption of bone structure in the donor site
- Donor site morbidity
- Allografting carries a risk of disease and/or infection
MSCs based Bone regeneration: Currently, the two ways that are being researched extensively are Hydrogel Scaffolds and Cell Surface Engineering.
1.HYDROGEL SCAFFOLD – Current scaffolds have incorporated biologically active materials along with mechanically stable materials to promote osteoinduction. This method includes seeding the scaffolds and hydrogels with MSCs and places the cells directly into the injury site to increase cell proliferation and lets them differentiate into osteoblasts which further get calcified, thus healing the bone.
2.CELL SURFACE ENGINEERING- There are naturally occurring receptors that are expressed on the surface of MSCs and all of them can potentially be used for cell targeting. These naturally occurring receptors may be effective in the direct transplantation of MSCs without prior changes. Some receptors promote MSC binding while some MSCs get modified to decrease their accumulation time in the bone marrow and so on. Different approaches are being used to enhance the proliferative ability and cell engraftment rates for bone regeneration and these reasons make Cell Surface engineering a very good prospect.
Why MSC based Regenerative Medicine a better option?
MSC-based bone regeneration is taken into account as an optimal approach because the current approach of delivering osteogenic cells onto the regeneration site includes the utilization of bone marrow aspirate from the iliac crest, which also contains growth factors. It is a minimally invasive procedure to enhance bone repair and produces satisfactory results. The different characteristics of MSCs make it possible to view them as a pioneer in regenerative medicine.
CONCLUSION
The capability of regeneration of damaged parts of the body to regain lost function has long been a dream of humanity. In recent years, extraction and optimization, and differentiation methods have allowed MSCs to progress closer to clinical applications for tissue reconstruction. Although MSCs have several advantages, there are still many challenges to beat. Many factors influence the potential of MSCs, such as induction factors, oxygen concentrations, and mechanical stimuli. Therefore, optimizing the culture conditions of MSCs may be an effective means to enhance the potential of MSCs. Despite the current challenges, MSC-based bone regeneration represents a promising clinical strategy in the field of regenerative medicine.
Reference (Aug-21-A4)

